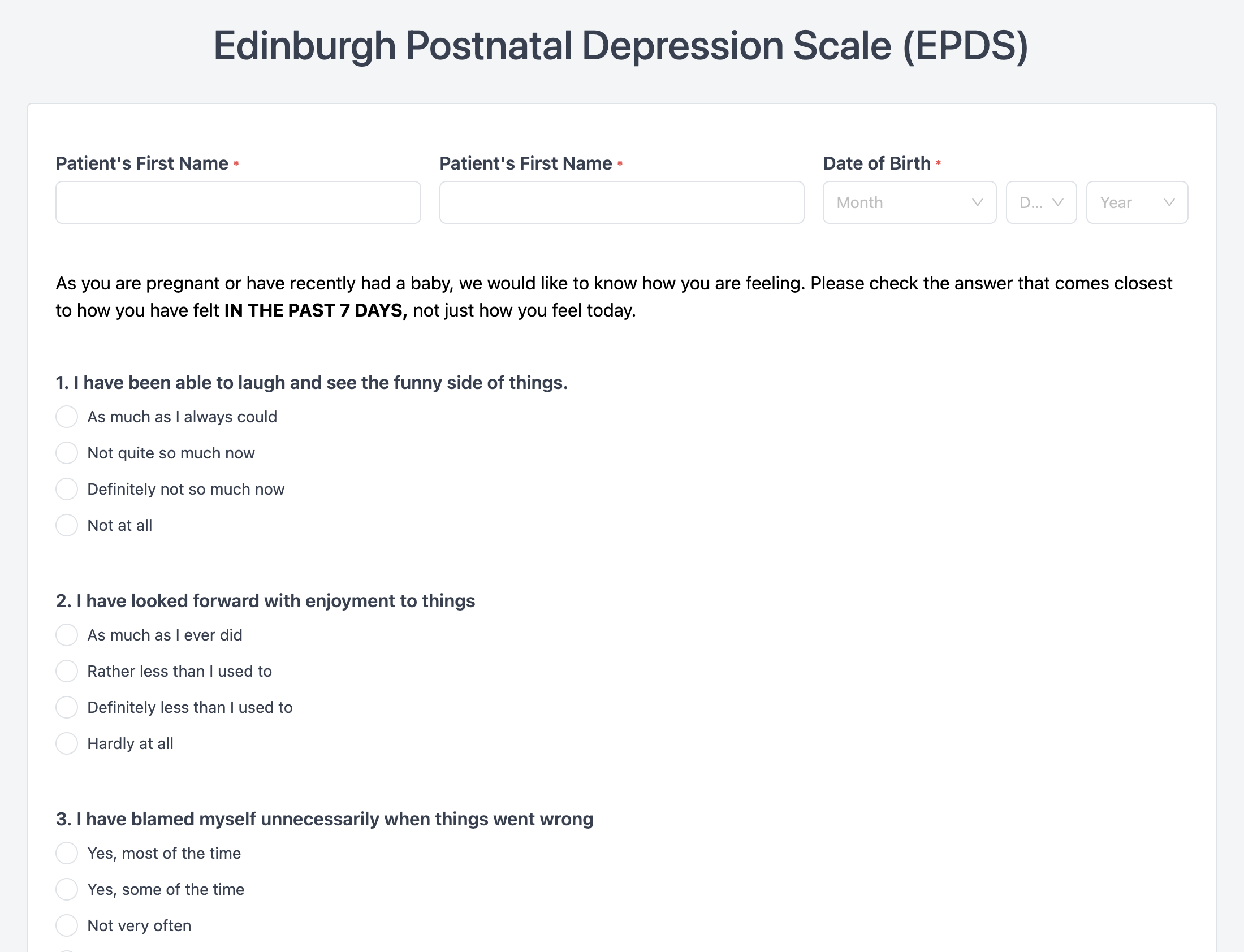

The Edinburgh Postnatal Depression Scale (EPDS) is a validated 10-item self-report questionnaire developed by J.L. Cox, J.M. Holden, and R. Sagovsky in 1987 to screen for postnatal depression in community and clinical settings. Each item is scored on a 4-point scale (0–3), yielding a total score of 0–30. A score of 10 or above is the recommended cutoff for broad screening programs, while a score of 13 or above indicates probable major depressive illness (Cox et al., 1987). The EPDS demonstrates good internal consistency (Cronbach's α = 0.79–0.87) and strong sensitivity (86%) and specificity (78%) at the 12/13 cutoff. Zentake's digital EPDS delivers the questionnaire via a HIPAA-compliant perinatal intake form and auto-calculates scores upon submission.
Each of the 10 items is rated on a scale of 0 to 3 (with response options varying by item — some are scored in reverse order). Sum all item scores for a total ranging from 0 to 30. Clinical interpretation ranges are:
Zentake automatically calculates the EPDS total score, flags scores at or above 10 for follow-up, and alerts clinicians to any non-zero response on Item 10 upon form submission.
Step 1: Introduce the questionnaire. Explain to the patient that the EPDS is a brief and confidential questionnaire about feelings over the past 7 days. Reassure her that responses will be used to provide better support. Zentake's digital intake platform delivers the EPDS automatically as part of the prenatal or postpartum visit workflow.
Step 2: Patient self-completes the 10-item questionnaire. The EPDS takes approximately 5 minutes and is designed for self-administration. Patients can complete it securely via Zentake's mobile-friendly form on a phone, tablet, or computer before or during the appointment.
Step 3: Review the auto-calculated score. Zentake instantly calculates the total score and flags whether it meets the screening threshold (10+) or probable depression threshold (13+). Clinicians can review results before entering the exam room.
Step 4: Conduct a clinical follow-up for positive screens. For scores of 10 or above, conduct a structured clinical interview to further assess depressive symptoms, risk factors, and functional impairment. For any non-zero Item 10 response, assess for suicidality immediately.
Step 5: Track scores longitudinally. ACOG recommends screening at the initial prenatal visit, later in pregnancy, and at postpartum visits. Zentake's longitudinal tracking enables comparison of EPDS scores across all perinatal encounters in a single dashboard.
Scoring: Paper EPDS requires awareness of reverse-scored items and manual summation; Zentake auto-calculates the total and flags threshold scores instantly with no clinician calculation required.
Completion: Paper forms can be completed incorrectly or skipped; Zentake's digital form validates all entries and ensures Item 10 is not overlooked.
Delivery: Paper requires printing, distributing, and collecting physical forms at each visit; Zentake sends the EPDS via secure link by text or email before the appointment, saving clinic time.
Data Storage: Paper forms must be scanned and filed; Zentake stores all responses securely in the cloud with automatic HIPAA-compliant audit trails.
Longitudinal Tracking: Manually comparing paper scores across prenatal and postpartum visits is cumbersome; Zentake's measures dashboard plots EPDS scores across all perinatal encounters for instant trend analysis.
Security: Paper forms containing sensitive mental health information can be misplaced; Zentake protects all data with 256-bit encryption and role-based access controls.
Integration: Paper data must be manually entered into the EMR; Zentake pushes completed EPDS results directly to the patient chart via EMR integration.
Cost: Paper forms incur printing, staff time, and storage costs; Zentake replaces these with an automated digital workflow at scale.
What does the EPDS measure?
The EPDS measures the presence and severity of depressive symptoms in the perinatal period (during pregnancy and up to 12 months postpartum). It screens for symptoms including depressed mood, anxiety, feelings of guilt, sleep disturbance, and thoughts of self-harm, but does not diagnose depression — a clinical interview is required for formal diagnosis.
How do you score the EPDS?
Sum the numerical scores for all 10 items, noting that some items are reverse-scored. Total scores range from 0 to 30. A score of 10 or above warrants clinical follow-up; 13 or above indicates probable major depression. Any non-zero response to Item 10 requires immediate clinical contact regardless of total score. Zentake auto-calculates scores and alerts clinicians to threshold results.
How long does the EPDS take to complete?
The EPDS typically takes 5 minutes or less to complete. It is specifically designed as a brief self-report tool that can be administered efficiently in busy perinatal clinic settings.
Is the EPDS free to use?
The original EPDS is in the public domain and freely available for clinical use. Zentake's digital EPDS template is included in all Zentake plans with no additional per-assessment licensing fees.
What age or population is the EPDS validated for?
The EPDS was originally validated for postpartum women but has since been validated for use during pregnancy (prenatal) as well as with fathers and partners experiencing perinatal depression. It is appropriate for adult perinatal populations across diverse cultural and linguistic groups, with validated translations available in over 60 languages.
Who should administer the EPDS?
The EPDS is designed for self-administration by the patient. It is appropriate for use in any perinatal clinical setting — obstetrics, midwifery, pediatrics, family medicine, and psychiatry. Clinicians should be prepared to follow up on all positive screens with appropriate clinical assessment and support.
When should the EPDS be administered?
ACOG recommends screening at the initial prenatal visit, once more during pregnancy, and at postpartum visits (typically 4–6 weeks and 6 months postpartum). Some guidelines recommend screening at every postpartum visit during the first year. Zentake enables automated scheduling of EPDS delivery at each of these touchpoints.
What should I do if a patient scores 13 or above on the EPDS?
A score of 13 or above indicates probable major depressive illness and requires immediate clinical assessment. This may include a structured clinical interview, safety planning, initiation of treatment (therapy or medication), and/or referral to a perinatal mental health specialist. Document all follow-up actions in the patient record via Zentake's EMR integration.
1. Cox JL, Holden JM, Sagovsky R. Detection of postnatal depression: Development of the 10-item Edinburgh Postnatal Depression Scale. British Journal of Psychiatry. 1987;150:782–786.
2. Gibson J, McKenzie-McHarg K, Shakespeare J, Price J, Gray R. A systematic review of studies validating the Edinburgh Postnatal Depression Scale in antepartum and postpartum women. Acta Psychiatrica Scandinavica. 2009;119(5):350–364.
3. Levis B, et al. Accuracy of the Edinburgh Postnatal Depression Scale (EPDS) for screening to detect major depression among pregnant and postpartum women: systematic review and meta-analysis. BMJ. 2020;371:m4022.
Last updated: March 2026